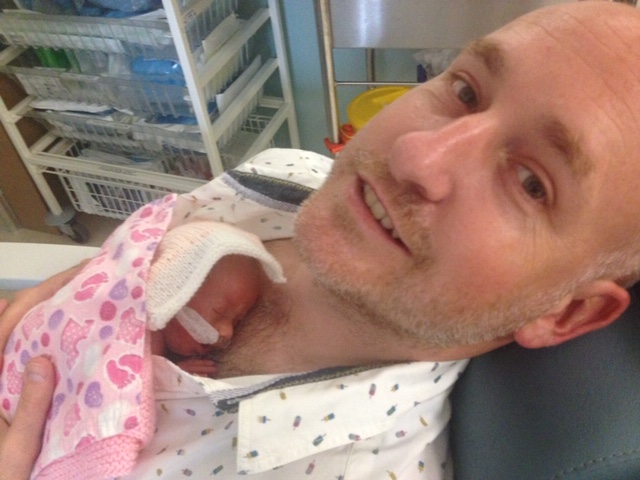
All pregnancies are precious, but ours was even more so for us because it came after years of trying to conceive, pregnancy losses and several cycles of IVF. It was only once I began feeling little kicks and flutters that I finally started to believe we’d have a baby at the end of it. Yet I didn’t realize that a grueling journey had only just begun for us.
At the 20 week scan, instead of finding out the sex of our baby we found out our poor baby had a huge cyst on the back of her head. We were referred to St. George’s Fetal Anomaly Unit where we learned that our baby had an Occipital Encephelocele; a very rare neural tube defect, affecting only 1 in 10,000 babies globally. Early in the pregnancy, the bottom of her skull had not completely closed up leaving a hole allowing cerebral fluid to leak out and potentially also brain tissue. The fluid build-up pushing on the skin around the back of the skull caused it to fill up like a balloon.
The prognosis for the baby was not good. Potential complications included seizures, blindness, and other physical and cognitive issues. That was if the baby survived at all. Devastation is not a big enough word for how we felt. We were faced with a terrible decision about whether to continue the pregnancy. We decided to wait until we had met with top geneticist, Dr. Tessa Homfray. Mercifully, she advised us to wait for the results of a MRI scan at 28 weeks before making any decisions as this would give us definitive answers.
However, by another weird twist of fate, we never had to make any decisions. At 27 weeks I suffered a nasty case of undiagnosed pre-eclampsia (or suspected eclampsia) and, to save both our lives, little Rosie was delivered via emergency c-section on 13th August 2017, weighing only 810g. I spent a week in intensive care myself and have no memory of any of this.
Rosie was transferred to St. George’s NICU with the complications of both the Encephalocele and extreme prematurity. This combination had not been experienced by any of the staff at the unit nor by the surgeon who would have to perform the essential surgery to remove the sac and close up Rosie’s head. It would be a first for the hospital, I believe.
Nevertheless, on day 9 the surgery could not wait any longer We were told the chances of Rosie surviving were not good; the risks of infection or blood loss were extremely high. We needed a miracle. That day was the longest, most surreal day of my life.
At 6pm we returned to the unit fearing the worst. As we walked past the nursery window, we saw that Rosie’s nurse had the biggest grin on her face. The surgery had been a success! There had only been fluid in the sac and now her head looked perfect with barely a scar. She was back in bed as if nothing had happened! That day we gave her the middle name: Hera – the Greek Goddess of Women, dedicated to her amazing strength. We are not religious people but we both said prayers of thanks that night and especially for the surgeon, Mr. Stapleton, and his team.
From then on, the focus was on keeping Rosie alive and thriving as a premature baby, which we learned was not always that easy. Every day for 7 weeks, we drove the 34 miles each way from West Sussex to Tooting. We held Rosie, changed teeny tiny nappies, stared at her sats monitor, experienced gut-wrenching moments, and just lived in the NNU bubble.
Rosie was in hospital for three months, (the last 6 weeks at our local one), finally coming home 3 days after her due date, tiny but healthy.
Rosie is now a happy, clever, chatty little girl, with no complications other than needing a shunt and delayed walking. She is thriving, all thanks to St. George’s NNU and First Touch!
Anna and Doug Goldfinch